If you have any skin problems, then chances are that your dermatologist may recommend a skin biopsy. It is a surgical procedure to diagnose skin problems to determine your skin condition for further testing or treatment plans. It has many forms and is generally safe to perform, however, sometimes complications can occur. Learn about excision lesion techniques for skin biopsy in this article. Please contact https://doralhw.org/department/dermatology/ for your queries.
What is a skin biopsy?
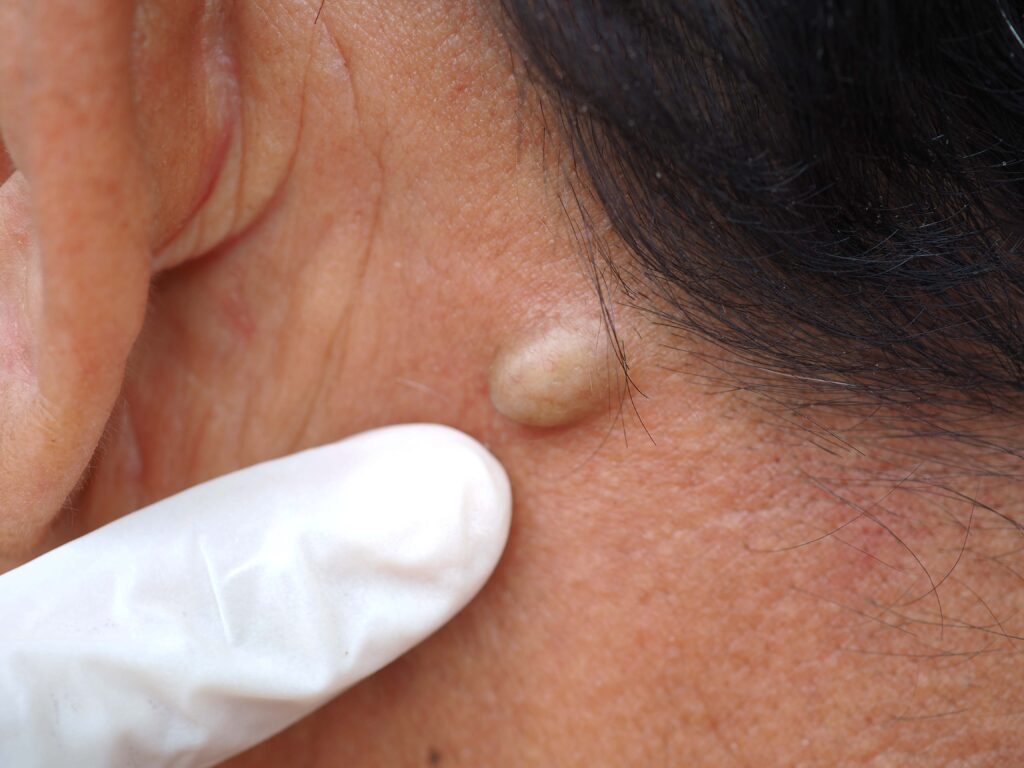
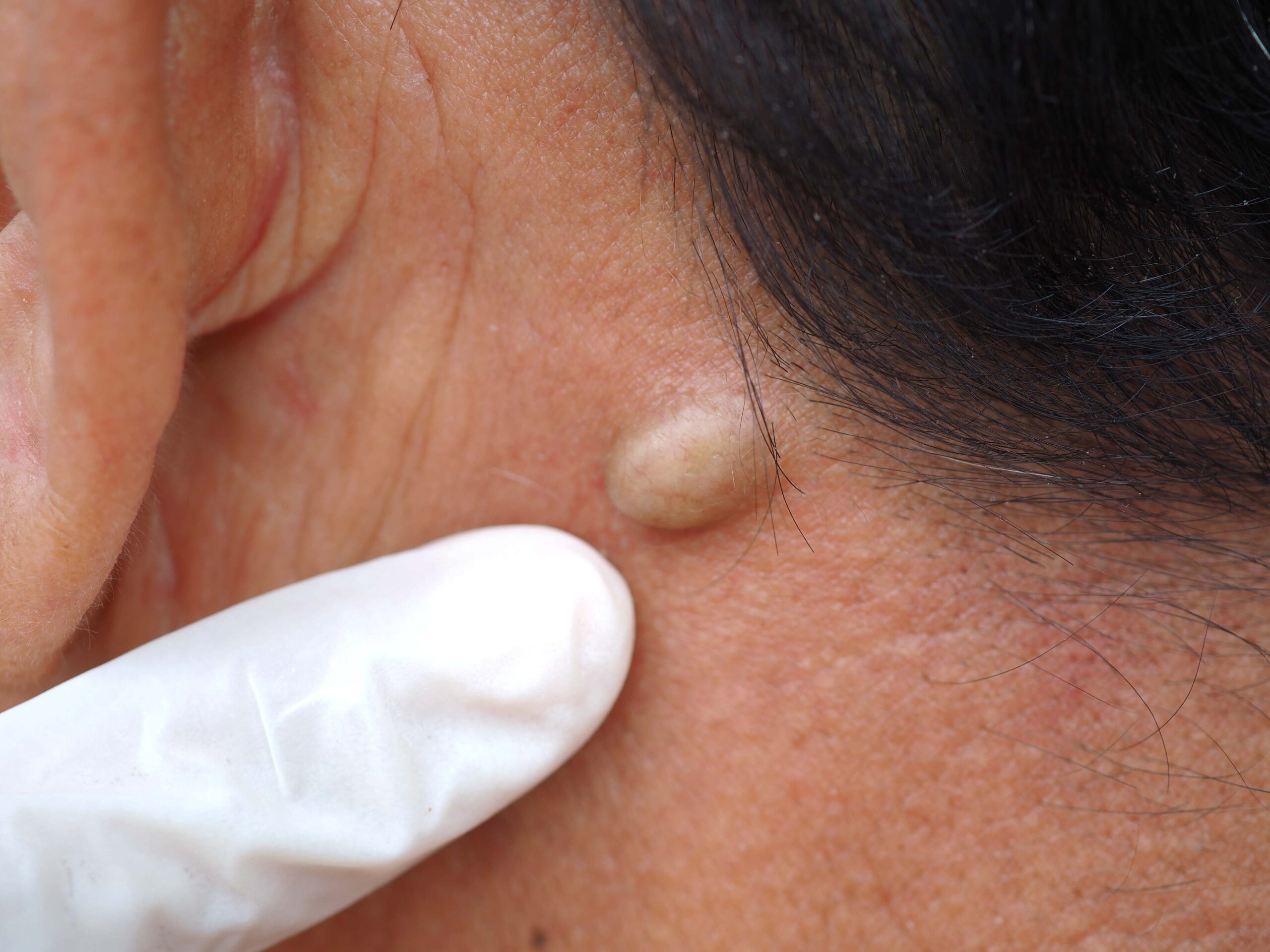
A skin biopsy is a diagnostic procedure where a small sample of skin is taken for testing. It is a safe and easy outpatient procedure. There are many methods to perform a skin biopsy depending on the size of the lesion, suspected clinical diagnosis, and site of the lesion.
To perform this procedure, the doctor injects a local anesthetic into the skin to numb the area. After they remove a sample of skin, it’s sent to the lab to be assessed under a microscope (to check for skin cancer/different skin conditions/skin infections). After the procedure, a suture or dressing may be applied to the site of the biopsy. Only some skin lesions need a biopsy. Most providers can diagnose many types of lesions just by seeing them.
Skin Biopsy Techniques
There are various techniques used for skin biopsy depending on the type of lesion, the site of the lesion, and also the expertise of the dermatologist. The most common techniques of skin biopsy are:
- Shave biopsy:
is a skin used to remove a sample of the skin’s top layers with a razor blade or scalpel (a small cutting blade used for surgery). The top layers of skin are called the epidermis and the dermis. No stitches are needed after the procedure, and the wound heals in 1 to 3 weeks. It may be used if the skin lesion is superficial or to confirm a diagnosis of intraepidermal carcinoma or basal cell carcinoma. The major drawbacks of this procedure are that it doesn’t include the full thickness of the skin and is difficult for a pathologist to identify invasive conditions.
It has a deep form of biopsy, called scoop biopsy, which removes the skin from a benign mole by scooping it out. It is also known as saucerization or tangential excision. This form of shave biopsy uses increased depth, which may lead to more extensive scarring if left to heal by secondary intention. In some cases, it may require stitches later on.
- Punch biopsy:
This biopsy is used to remove a small section of skin, including deeper layers, with the help of a special tool with a round blade to remove the skin sample. It is used to extract skin tissue from layers called the epidermis, the dermis, and the top layer of fat under the skin. It is the most used biopsy, which is quick to perform and leaves a small wound that needs to be stitched.
This biopsy gives a good overview of the skin tissue layer for a pathologist to rule out the disease that involves deep layers of the skin. The doctor uses a disposable skin biopsy punch, which has a round stainless-steel blade ranging from 2 to 6 mm in diameter, to remove 3 to 4 mm of skin. The doctor holds the instrument at a 90-degree angle to the skin and rotates it to cut the skin, using forceps and scissors on the skin sample to completely remove it. A suture may be used to close the wound or stop bleeding. If the wound is too small, it may heal without sutures.
- Excisional biopsy:
This biopsy is used to remove all of the skin lesions, including the entire lump or an area of irregular skin, with the help of a scalpel. This skin sample includes the full thickness of the skin along with the fat below the skin. This biopsy may remove a border of healthy skin to improve the chances of complete removal. Smaller lesions are mostly removed by using a scalpel blade in an elliptical motion, with some closure sutures. Larger excisions may be repaired with a skin flap (moving adjacent skin together to cover the wound) or graft (skin taken from another site to patch the wound).
- Incisional biopsy:
This biopsy is used to remove a larger or deeper ellipse of skin by using a scalpel blade. Usually, stitches are required after the procedure. It is used to confirm the diagnosis when inflammatory dermatosis is suspected. It may remove some of the surrounding healthy skin. It provides a better overview for the pathologist to get better diagnostic results. It can be helpful when deeper layers of tissue involved in the disease process are removed like subcutaneous fat or medium-sized blood vessels.
Complications of Skin Biopsy
Skin biopsy is usually a safe procedure, however, sometimes complications can occur. This often can happen when a larger skin sample is removed. The complications that might occur include:
- Bleeding: Intraoperative or postoperative bleeding can occur in anyone, but mostly in individuals who have bleeding problems or take blood-thinning medications like warfarin or aspirin.
- Infection: Bacterial wound infection can occur in 1 to 5% of excisional biopsies. However, it is exceedingly rare in small punches, shaves, or incisional biopsies. Factors like skin lesions with ulcers or crusting on them, site of biopsy, patient’s existing health conditions like diabetes, older age, or use of immunosuppressive medicines can increase the risk of infection.
- Nerve injury: Sometimes, the blade may cut a superficial sensory nerve that causes pain or numbness. It may occur when the skin is thin, for example, on the face or back of the hand. The risk of impairing motor nerves is extremely rare but can occur during skin cancer surgery in facial danger zones, areas supplied by the temporal, marginal mandibular, and zygomatic branches of the facial nerve and spinal accessory nerve.
- Scarring: This can occur at the biopsy site and may leave a permanent scar. Some of the most common body sites for scarring are the center of the chest (a common site for excessive or hypertrophic scars). Most common among Afro-Caribbean skin types.
- Persistence or recurrence of the skin lesion: Many biopsies are partially or only intended for diagnostic purposes. Excisional biopsies involve a risk of not removing the full lesion, which may recur afterward.
- Anesthetic problems: Some people are allergic to local anesthetics and may develop a vasovagal reaction, which may cause the patient to faint or potentially hurt the individual. Palpitations are another side effect that is related to the adrenaline used in the local anesthetic.
- Wound breakdown: It is an uncommon complication of sutured wounds and occurs when biopsy sites have a lot of tension, increasing the risk of scar formation, like the chest or back, immediately after suture removal or result of infection. To prevent this, avoiding exercise or the use of strapping and dissolvable sutures may help.
Results of Skin Biopsy
Results can take one to two weeks to come after the pathologist examines your skin sample for clinical diagnosis. If your result shows no cancer or skin disease, then your result is normal. If your result is positive for cancer or a specific skin condition, it means your result is abnormal and you may need more tests to find out the condition you have. Sometimes your results may not be clear; in that case, your doctor tells you to get a biopsy again or may recommend other tests.
Excision lesion techniques like shave, punch, excisional, and incisional biopsy are used to diagnose skin cancer or other skin conditions that cause your symptoms. It helps the doctor determine the skin condition you have and what further testing or treatment you need to improve your skin condition.
Need help with skin problems? Visit our dermatology clinic in Brooklyn to get professional medical help or for cosmetic purposes. Call us to book your appointment now!!!! At Doral Health and Wellness Dermatology Center, we have the best dermatologists who can help you take care of your skin. As dermatology experts in East New York, we provide the best services. You can visit us at 1797 Pitkin Avenue, Brooklyn, New York to schedule an appointment. You can also call us at +1-718-367-2555 or visit our website at https://doralhw.org/department/dermatology/ .