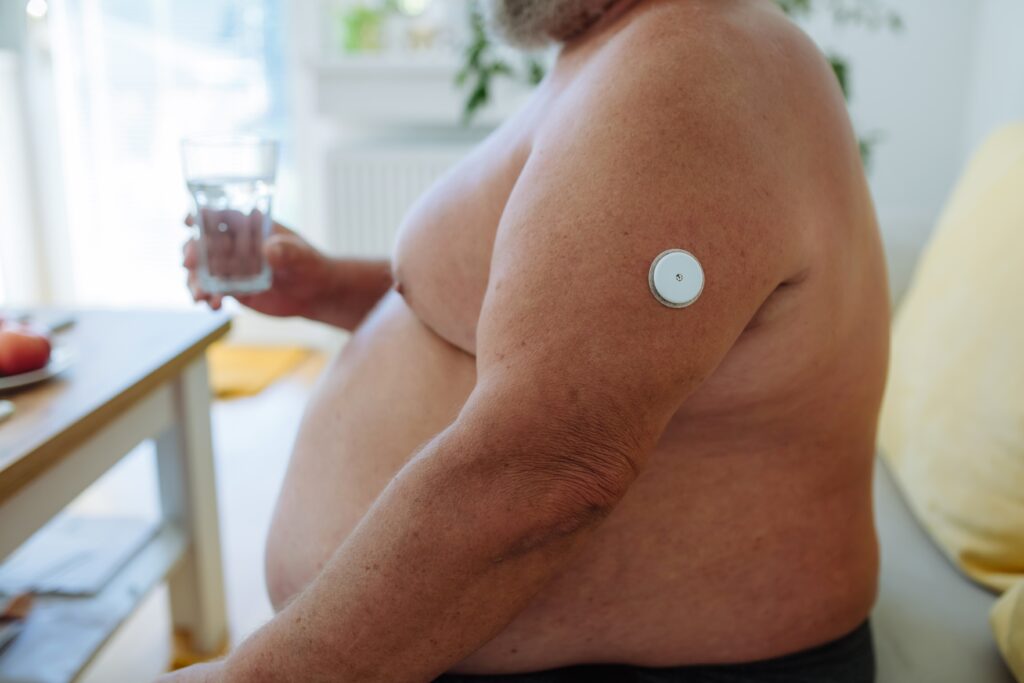
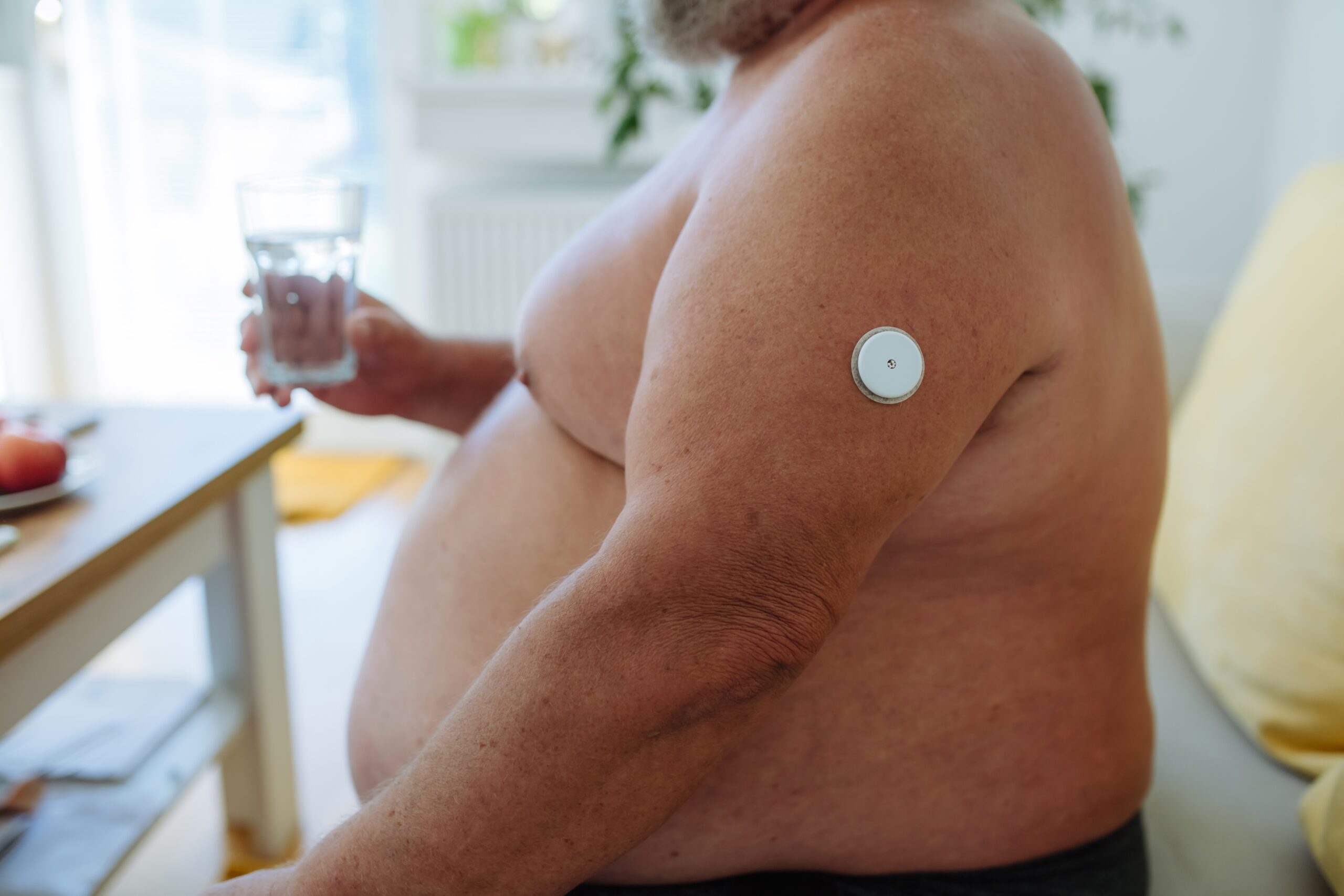
Did you know that your daily water intake can directly influence your glucose levels? The relationship between hydration and blood sugar is often overlooked, but it’s essential to maintaining your overall health. Proper hydration supports your body’s ability to balance glucose by aiding the transport of sugar into your bloodstream and helping the kidneys eliminate excess glucose through urine.
When you’re not drinking enough water, your body struggles to maintain this balance. Dehydration leads to more concentrated blood, which can cause blood sugar levels to rise. Over time, this may contribute to insulin resistance or even elevate your risk of developing chronic conditions like type 2 diabetes. That’s why understanding how hydration and blood sugar work together is critical for prevention and daily glucose control.
Maintaining good hydration habits is one of the simplest and most effective ways to support healthy metabolic function. Whether you’re already managing a condition or simply looking to improve your well-being, keeping your fluid intake consistent can make a major difference in how your body handles sugar.
To learn more about the science behind hydration and blood sugar, and how improving your water intake can positively impact your health, read the full article on our website. Take the first step toward a healthier you—visit www.doralhw.org today and book a consultation with our medical experts.
The link between Hydration and Blood Sugar
Hydration plays a crucial role in managing blood sugar levels. As you know, our body is 50 to 70% water. It ensures that the amount of glucose entering your bloodstream is relative to the amount of overall liquid that makes up your blood. When you’re metabolically healthy, your body is in a state of osmotic homeostasis, which means maintaining a balance of fluids constantly throughout the body. Your body achieves this through hormones, such as vasopressin, and your thirst response, so you can intake sufficient water.
However, in case you’re diabetic, your body will struggle to manage water levels, which leads to elevated levels of sugar in your blood and urine. High blood sugar, also known as hyperglycemia, causes dehydration as its first sign because the body tries to remove excess glucose through your urine. That’s why frequent urination is a common sign of diabetes. Dehydration can make your blood more concentrated and may alter hormones like insulin that manage blood sugar. Some research suggests that dehydration can lead to diabetes over time, while more research is needed to confirm this link.
You need to ensure that you drink enough water to prevent dehydration and manage moderate spikes in blood sugar if you have diabetes or prediabetes. Current research shows that drinking more water creates different short and long-term effects, and these effects impact blood sugar differently. But this confirms that consuming enough water is necessary to manage blood sugar levels, especially if you’re diabetic or have prediabetes.
Signs You Aren’t Drinking Enough Water
Staying well-hydrated is essential for your energy, focus, and metabolic health. When your body doesn’t get enough fluids, it begins to show warning signs that shouldn’t be ignored. The connection between hydration and blood sugar becomes especially important here—dehydration not only makes you feel sluggish but can also affect how your body regulates glucose.
Here are several signs that you might be dehydrated:
- Dark yellow urine – This is one of the earliest and most visible signs. The darker your urine, the more dehydrated you may be. Poor hydration can make it harder for your kidneys to filter excess glucose, reinforcing the link between hydration and blood sugar regulation.
- Dizziness, lightheadedness, or fatigue – These symptoms often occur when blood volume drops due to dehydration, affecting oxygen and glucose delivery to your brain and muscles.
- Nausea – Even mild dehydration can trigger gastrointestinal discomfort. It can also interrupt your body’s natural process of glucose balance, highlighting how hydration and blood sugar are tightly connected.
- Muscle cramps – Water helps your muscles function properly. When hydration is low, cramps are more likely, especially during exercise. This imbalance can also stress your body’s ability to manage energy, including blood sugar levels.
- Frequent headaches – Headaches can stem from both dehydration and glucose fluctuations. In fact, dehydration-related headaches are often worsened by poor blood sugar control, further emphasizing the relationship between hydration and blood sugar.
- Dry mouth – Saliva plays a role in digestion and overall health. A dry mouth can signal both dehydration and imbalanced glucose levels.
Understanding these signs is critical for preventing bigger issues. If you regularly experience any of these symptoms, your water intake might be too low—and that could be affecting your hydration and blood sugar balance more than you think. Drinking adequate water throughout the day supports your body’s ability to process glucose efficiently and maintain overall well-being.
Staying Hydrated the Smart Way
Managing hydration and blood sugar becomes especially important during hot weather—especially for individuals with diabetes or prediabetes. High temperatures and direct sunlight can amplify the effects of dehydration, placing additional stress on your body’s ability to maintain stable glucose levels. Fortunately, with a few practical strategies, you can protect yourself from dehydration-related complications and support better blood sugar control.
1. Choose the Right Fluids
The first step to maintaining proper hydration and blood sugar levels is choosing fluids that hydrate you without spiking your glucose. Focus on drinking water, seltzer, and unsweetened beverages like sugar-free lemonade or herbal teas. Avoid sugary drinks, caffeinated beverages, and alcohol, as they can worsen dehydration and cause your blood sugar to fluctuate. Drinking consistently throughout the day, rather than waiting until you feel thirsty, is key to protecting your overall balance.
2. Recognize and Prevent Heat Exhaustion
People with diabetes are more vulnerable to heat-related illnesses. Whether you’re walking, working, or just relaxing outdoors, always be alert to signs of heat exhaustion: dizziness, muscle cramps, intense sweating, fainting, headaches, nausea, or a racing heartbeat. These symptoms not only signal physical distress but also affect your hydration and blood sugar regulation. If you or someone you care for shows these signs, act quickly—move to a shaded or air-conditioned area, hydrate with cold fluids, and seek medical attention if symptoms persist.
3. Modify Your Exercise Routine
Physical activity is vital for managing hydration and blood sugar, but timing and setting matter. Avoid working out during peak heat hours. Instead, exercise indoors or early in the morning when temperatures are more manageable. This helps reduce the risk of overheating and ensures your body maintains better hydration levels, preventing sudden spikes or drops in blood sugar caused by physical stress and fluid loss.
4. Keep a Closer Eye on Your Glucose
In hot weather, blood sugar levels can fluctuate more than usual. That’s why it’s essential to monitor your glucose at least four times daily—or even more frequently if you’re active outdoors. Heat can cause insulin to act differently and may affect how your body absorbs glucose. Keeping your body hydrated helps stabilize these changes. Maintaining your hydration and blood sugar becomes even more effective when you pair regular monitoring with strategic snacking and consistent fluid intake throughout the day.
5. Store Insulin and Supplies Properly
Extreme temperatures can damage insulin and blood sugar testing supplies. Never leave insulin pens, test strips, or glucose meters in your car or exposed to direct sunlight. Instead, carry them in a temperature-controlled bag or cooler pouch. Remember, proper storage isn’t just about preserving your supplies—it directly impacts how well you can manage your hydration and blood sugar when you need it most.
By understanding how heat affects both hydration and blood sugar, and taking proactive steps to adjust your routine, you can stay safe, feel better, and avoid unexpected health issues. If you’re unsure how to manage your hydration and glucose levels during summer, contact us at www.doralhw.org to schedule a personalized consultation.
What to do in an emergency?
If you have diabetes or know someone who does, it’s crucial to understand what you should do if blood sugar gets dangerously high. If possible, get a blood glucose test or check the signs of high blood sugar or hyperglycemia, such as:
- Need to pee frequently
- Feeling thirstier than usual
- Feeling tired or weak
- Having headaches
- Having blurred vision
If you have type 2 diabetes or hyperglycemia, follow these steps to manage it:
- Take your insulin: First, make sure you take your insulin or other medication as prescribed by your doctor. It may be enough to lower your blood sugar to a safer range.
- Move your body: Moderate-intensity exercise, like brisk walking, will lower your blood sugar levels. Make sure you avoid high-intensity exercise because it temporarily raises your level.
- Stay hydrated: You may need to drink more water than usual to ensure your body gets rid of excess sugar in your urine.
- Call an ambulance: If you’re feeling drowsy or confused, or like you may be losing consciousness, call emergency services immediately.
Hydration and blood sugar are closely connected because a sufficient amount of water is required to maintain blood sugar levels in the body. If your water intake is not sufficient or you get dehydrated, your risk of developing hyperglycemia or making it worse is possible. So, make sure you drink enough water to prevent dehydration and manage your blood sugar levels to prevent serious complications. Follow the above-mentioned tips to stay hydrated to manage blood sugar levels this summer.
If you need help with diabetes or prediabetes, visit our diabetes specialist in the Brooklyn clinic to get professional medical help. Reach out to us to book your appointment now!!!!! Call us on +1-718-367-2555 and get answers for all your queries. Log on to www.doralhw.org or visit us at 1797 Pitkin Avenue, Brooklyn, NY 11212 to book an appointment with our endocrinologist to get the best treatment. We have the best endocrinologists who treat all endocrinal disorders and helpful staff to aid you during your treatment.