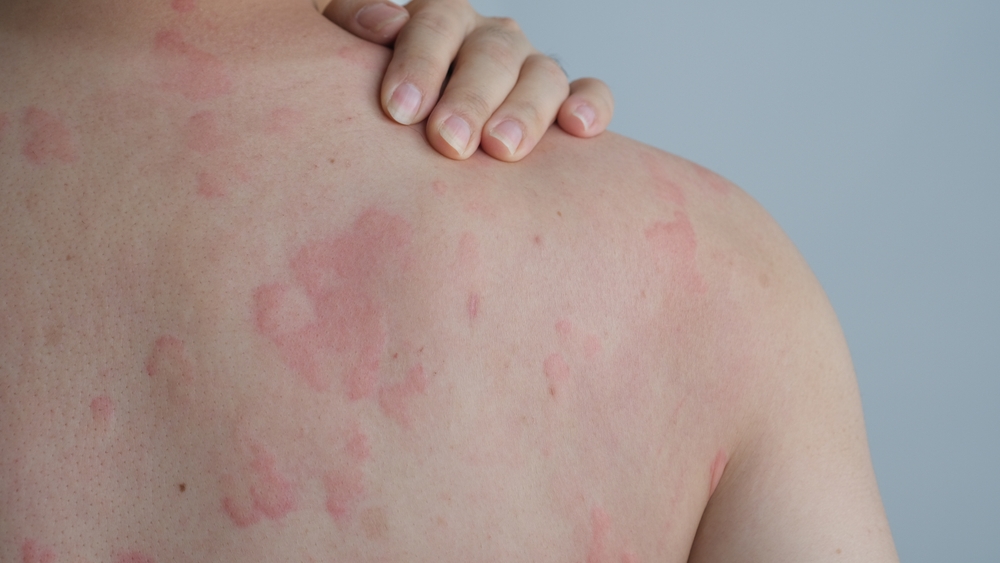
Hives can appear on your skin suddenly, leaving you with itchy, raised welts and a lot of questions. Understanding the reason hives (urticaria) appear on your skin involves looking at the complex immune response happening just beneath the surface. While there are many potential urticaria causes, the underlying mechanism is a fascinating process driven by your body’s defense system. This article will break down the science behind hives, explaining what happens inside your body to trigger this common and often frustrating skin reaction. At Doral Health & Wellness, we have all the answers you need.
Hives, or urticaria, are a sign that your immune system has been activated. The welts themselves are a direct result of specific cells releasing chemicals into your skin. By understanding this process, you can better manage your symptoms and work with a specialist to identify your triggers.
The Central Role of Mast Cells and Histamine
At the heart of every hive outbreak are specialized immune cells called mast cells. These cells are found in your skin, lungs, gut, and other tissues that come into contact with the outside world. Think of them as tiny, first-responder soldiers, armed and ready to defend your body against perceived threats.
So, what is the reason for hives (urticaria) appearing on your skin? It begins when a trigger—be it an allergen, a physical stimulus, or even stress—activates these mast cells.
The Triggering and Degranulation Process
- Activation: When your body is exposed to a trigger, your immune system may produce an antibody called Immunoglobulin E (IgE). This IgE antibody attaches itself to the surface of mast cells.
- Cross-linking: The next time you encounter that same trigger, it binds to the IgE antibodies on the mast cells, creating a bridge or “cross-link” between them.
- Degranulation: This cross-linking signals the mast cells to “degranulate,” which means they instantly release their contents. These contents include powerful inflammatory chemicals, the most famous of which is histamine.
The Effect of Histamine Release
Once released, histamine gets to work immediately. It has two primary effects that lead to the classic symptoms of hives:
- Vasodilation: Histamine causes small blood vessels in your skin to widen or dilate. This increases blood flow to the area, which is why hives appear red and feel warm.
- Increased Permeability: It also makes the walls of these blood vessels more permeable, or leaky. This allows fluid from the bloodstream to seep into the surrounding skin tissue, causing the swelling and raised welts (wheals) characteristic of hives.
Histamine also stimulates nerve endings in the skin, which sends a signal to your brain that you interpret as an intense itch. This entire chain reaction can happen within minutes of exposure to a trigger.
Exploring the Common Urticaria Causes
The mechanism involving mast cells and histamine is the final common pathway for all types of urticaria. However, the initial triggers can be incredibly diverse. Identifying these triggers is a key part of management.
Allergic Urticaria
This is what most people think of when they hear about hives. The immune system overreacts to a harmless substance. Common triggers include:
- Foods (like shellfish, nuts, and eggs)
- Medications (such as antibiotics and aspirin)
- Insect stings or bites
- Environmental allergens (like pollen or pet dander)
Physical Urticaria
In some cases, the trigger is not a substance but a physical stimulus. The mast cells are directly stimulated by environmental factors. Examples include:
- Dermatographia: Hives form after scratching or stroking the skin.
- Cold Urticaria: A reaction to cold exposure.
- Cholinergic Urticaria: Triggered by an increase in body temperature from exercise, hot showers, or stress.
- Pressure Urticaria: Caused by prolonged pressure on the skin, such as from tight clothing.
Idiopathic and Autoimmune Urticaria
For many people with chronic hives (lasting more than six weeks), a specific external trigger is never found. This is called chronic idiopathic urticaria (CIU). In a significant portion of these cases, the condition is actually autoimmune. The body mistakenly produces antibodies that directly activate the mast cells, even without an external trigger.
When to Consult a Specialist for Urticaria
If your hives are frequent, severe, or last for more than a few days, it’s important to seek professional help. An allergist is a medical doctor who specializes in diagnosing and treating conditions like urticaria. They can help investigate potential triggers and create an effective treatment plan.
For those with persistent or complex symptoms, visiting a specialized immunology clinic in Brooklyn can provide access to advanced diagnostic testing. An allergist at such a facility can determine if your chronic hives might have an autoimmune component and recommend more targeted therapies. A specialist at an immunology clinic in Brooklyn will have the expertise to manage even the most challenging cases.
The goal of treatment is to block the effects of histamine with antihistamines or, in more severe cases, to stabilize the mast cells or modulate the immune system.
In essence, hives are an external sign of an internal immune event. The release of histamine from mast cells leads to leaky blood vessels, causing the tell-tale welts and itch. By understanding this mechanism, you and your doctor can work together to control your symptoms and improve your quality of life. Call us on + 1-718-367-2555 to book your appointment now to receive the best-in-class treatment that helps manage your allergies for a better life. Take action now, before it’s too late! If you need help, register your information at https://yuz88hfiyh7.typeform.com/Doralintake. Or visit us at 1797 Pitkin Avenue, Brooklyn, NY 11212.