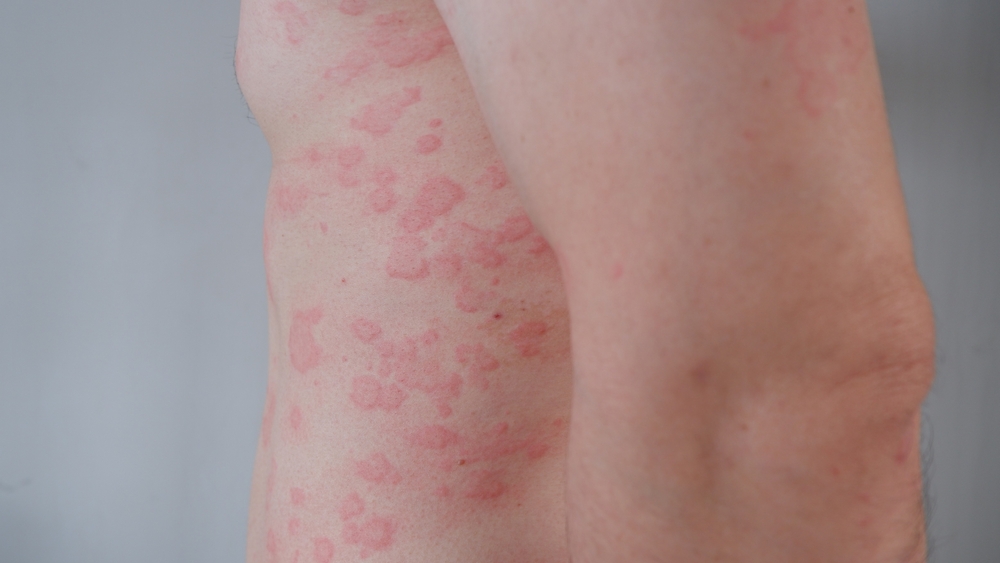
Dealing with hives can be a frustrating and uncomfortable experience. The sudden appearance of itchy, red welts on the skin often leaves people searching for answers. Understanding the common causes of hives is the first step toward finding relief. This guide provides a detailed overview of hives (urticaria) causes and management, helping you identify potential triggers and explore effective strategies for treatment. Effective hives management begins with knowledge, empowering you to take control of your skin health.
Hives, or urticaria, are a common skin reaction affecting about 20% of people at some point in their lives. They can be classified as acute (lasting less than six weeks) or chronic (persisting longer than six weeks). Identifying the root cause is key to preventing future outbreaks. At Doral Health & Wellness, we have all the answers you need.
The triggers for hives can be incredibly varied, ranging from allergic reactions to physical stimuli. While it’s not always possible to pinpoint a single cause, especially in chronic cases, knowing the potential culprits is essential for effective management.
Allergic Reactions
Allergies are one of the most frequent causes of hives. When your body encounters a substance it perceives as a threat, it releases histamine and other chemicals into the bloodstream, leading to the characteristic welts. Common allergens include:
- Foods: Nuts, eggs, shellfish, milk, and certain fruits are well-known triggers.
- Medications: Antibiotics (especially penicillin), aspirin, ibuprofen, and some blood pressure medications can cause hives.
- Insect Stings or Bites: Reactions to bees, wasps, and fire ants are common.
- Pollen and Pet Dander: Inhaled allergens can sometimes manifest as skin reactions.
Infections
Both viral and bacterial infections can trigger hives as your immune system mounts a response. These include:
- The common cold or flu
- Strep throat
- Urinary tract infections (UTIs)
- Hepatitis
In these cases, the hives usually resolve as the underlying infection is treated and clears up.
Physical Triggers (Physical Urticaria)
Sometimes, hives are caused by direct physical stimulation of the skin. This is known as physical urticaria and can be prompted by:
- Pressure: Tight clothing, belts, or even sitting for a long time can cause welts.
- Temperature Changes: Exposure to cold (cold urticaria) or heat can trigger a reaction.
- Sunlight: Solar urticaria is a rare condition where sun exposure causes hives.
- Exercise: An increase in body temperature from physical activity can lead to cholinergic urticaria.
- Water: In extremely rare cases, contact with water, regardless of temperature, can cause hives (aquagenic urticaria).
Other Potential Causes
Chronic hives are often idiopathic, meaning no specific cause can be found. However, they are sometimes linked to underlying autoimmune conditions like lupus or thyroid disease. Stress is also a significant contributing factor, as it can exacerbate existing conditions and trigger outbreaks.
Effective Hive Management Strategies
The primary goal of hives management is to relieve symptoms and prevent new welts from forming. The approach depends on whether your hives are acute or chronic.
At-Home and Over-the-Counter Treatments
For mild, acute cases, several simple measures can provide relief:
- Antihistamines: Non-drowsy, over-the-counter antihistamines like cetirizine or loratadine are the first line of defense. They work by blocking histamine, the chemical responsible for itching and swelling.
- Cool Compresses: Applying a cool, damp cloth to the affected areas can soothe itching and reduce inflammation.
- Avoid Triggers: If you know what caused your hives, do your best to avoid it. This might mean changing your diet, laundry detergent, or soap.
When to See a Specialist
If your hives are severe, persist for more than a few days, or recur frequently, it’s time to seek professional medical advice. A primary care doctor may refer you to a specialist. An allergist is an expert in diagnosing and treating allergic conditions, including urticaria. They can perform tests to identify specific triggers that might not be obvious.
For those with persistent or complex cases, a specialized facility like an immunology clinic in Brooklyn can offer advanced diagnostic tools and treatment plans. These clinics are equipped to handle chronic idiopathic urticaria and cases linked to autoimmune disorders. A specialist at an immunology clinic in Brooklyn can provide a comprehensive approach to your care.
Prescription Medications and Advanced Therapies
If over-the-counter options are not enough, your allergist may recommend stronger treatments. This could include:
- Prescription-strength antihistamines or a combination of different types.
- Corticosteroids, like prednisone, are used for short-term use to control severe flare-ups.
- Biologic medications, such as omalizumab, are given by injection for chronic idiopathic urticaria that doesn’t respond to antihistamines.
Managing hives effectively requires a partnership between you and your healthcare provider. By identifying triggers and following a consistent treatment plan, you can significantly reduce the impact of hives on your daily life. Call us on + 1-718-367-2555 to book your appointment now to receive the best-in-class treatment that helps manage your allergies for a better life. Take action now, before it’s too late! If you need help, register your information at https://yuz88hfiyh7.typeform.com/Doralintake. Or visit us at 1797 Pitkin Avenue, Brooklyn, NY 11212.